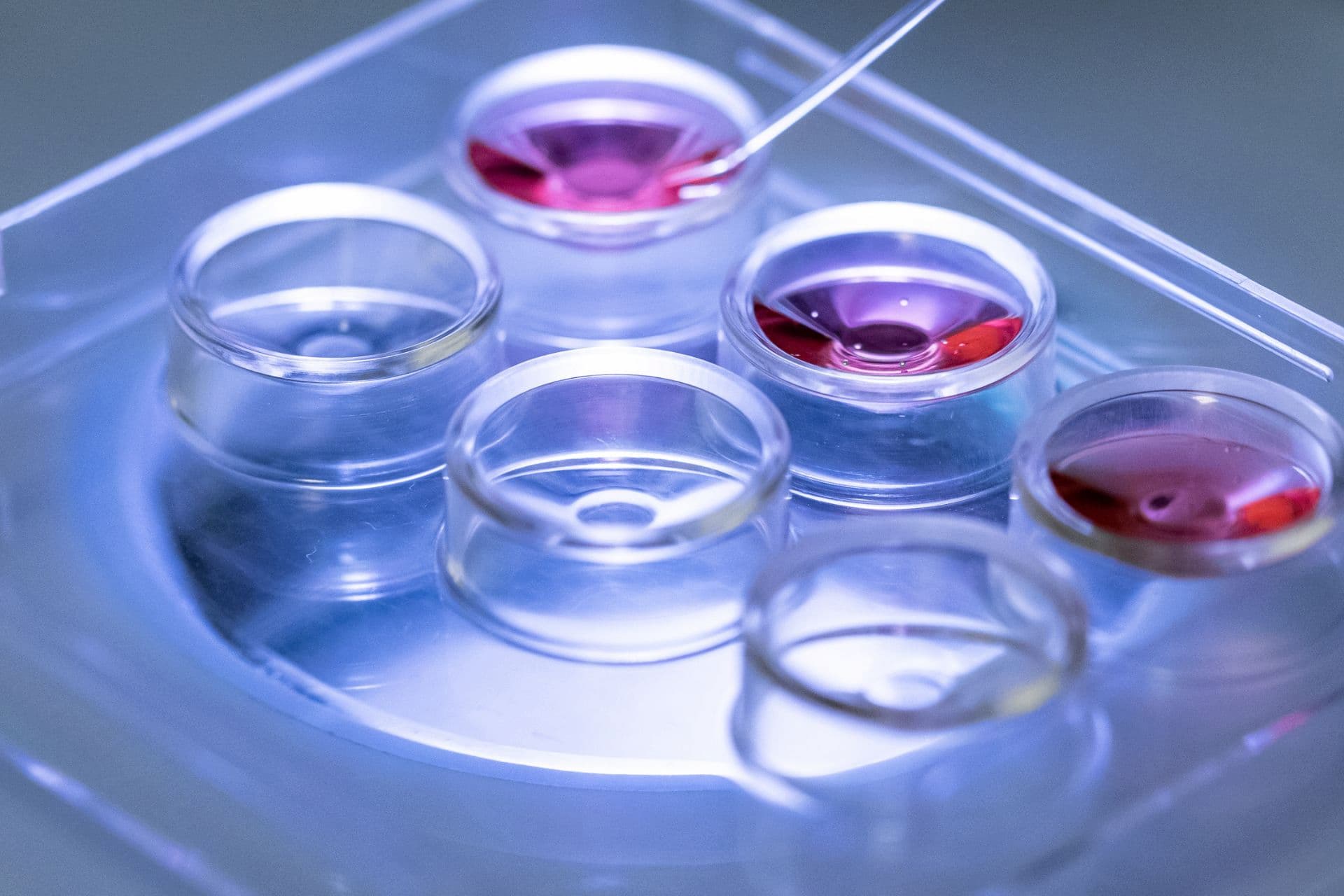
Share your eggs and share the gift of life
Become an egg share donor during your IVF treatment and help someone else become a parent.
Introduction
Is egg sharing right for me?
You’ll understand more than most that everyone’s fertility journey is unique. For some women, their only chance at having a baby of their own is by using donated eggs. That’s why we offer a unique egg sharing programme that gives women the chance to help each other. As an egg share donor, there’s no charge for your IVF treatment, while your recipient will get the precious eggs they need for IVF.
Who’s it for
You might want to become an egg share donor if…
- You’re between 18 and 35
- You want to save money on your IVF treatment
- You’re a non-smoker
- You’re fit and healthy with a BMI between 20 and 30
- You have a good ovarian reserve
- You have a normal baseline FSH level (less than 10 IU/L)
- You have both ovaries in place
- You have no history of severe endometriosis
- You have no genetic illnesses
- You have a good ovarian reserve – don’t worry: we will check this for you
Statistics at Harley Street
We’ve helped many partners, individuals and LBGTQ+ couples start their family since we opened our clinic in 2010 and we have some of the highest success rates for IVF in the country.

The egg sharing process and what to expect
Step 1: Assessment
We put every patient on the best possible treatment plan with the highest chance of success. That process starts with our thoughtful and thorough screening, which is focused on understanding you and your fertility health. As an egg sharer, this also includes a medical history form.

Step 2: Counselling
Sharing your eggs is a wonderful gift for another, but there are also a lot of social and ethical issues to think about. You’ll have the chance to talk about them all during an implications counselling session with our accredited fertility counsellor.

Step 3: Screening
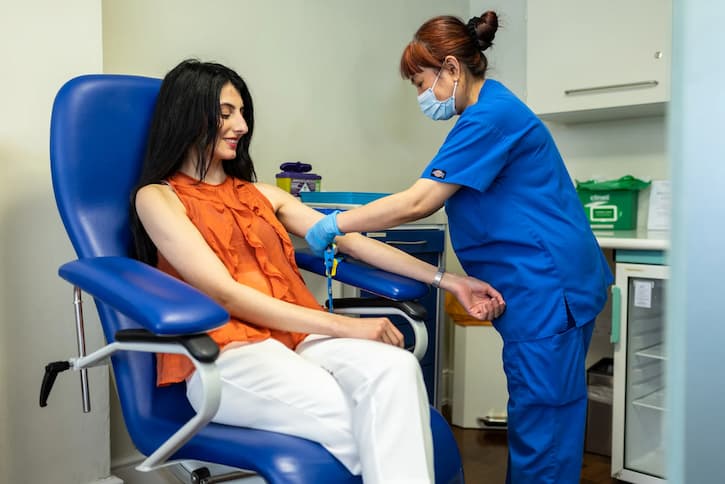
Step 4: Preparing for treatment
Once you have completed the screening, you’ll have a pre-treatment nurse consultation. Our team will go over your treatment plan, book in your appointments and answer any questions you may have.
You’ll typically be asked to take some tablets to prime your ovaries for stimulation before your cycle starts.

Step 5: Stimulating your ovaries
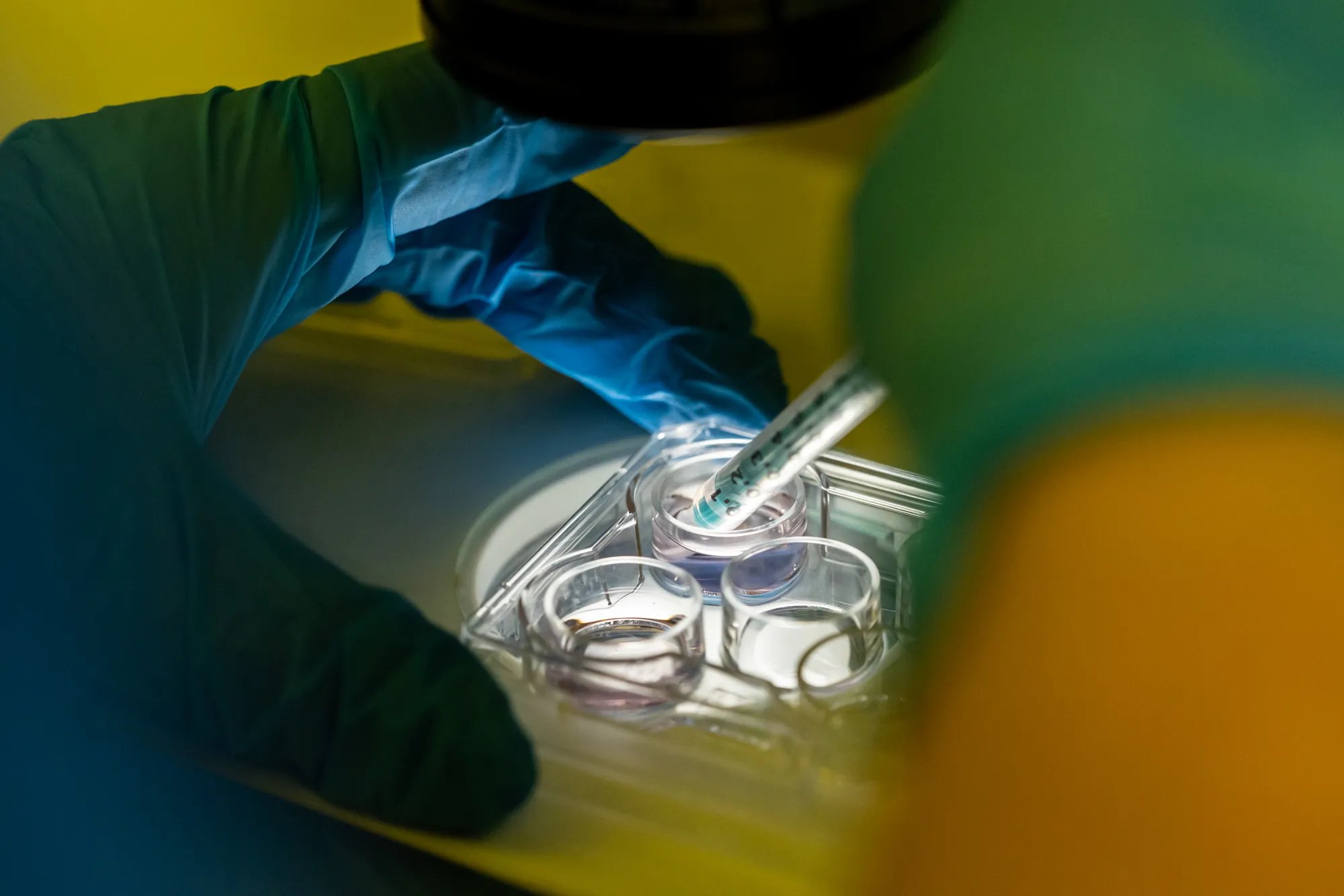
Step 6: Monitoring
Ideally, we’ll see 10 to 14 good-sized follicles on the ultrasound scan. If there are fewer than 10 you have a few options:
- Donate the first five eggs and keep any remaining eggs for yourself.
- Donate all the eggs and have a subsequent free IVF cycle for yourself.
- Opt out of the egg sharing treatment, continue the treatment and keep all the eggs collected. You’ll be charged for IVF treatment at current prices.
- Abandon the cycle with no further cost or commitment.
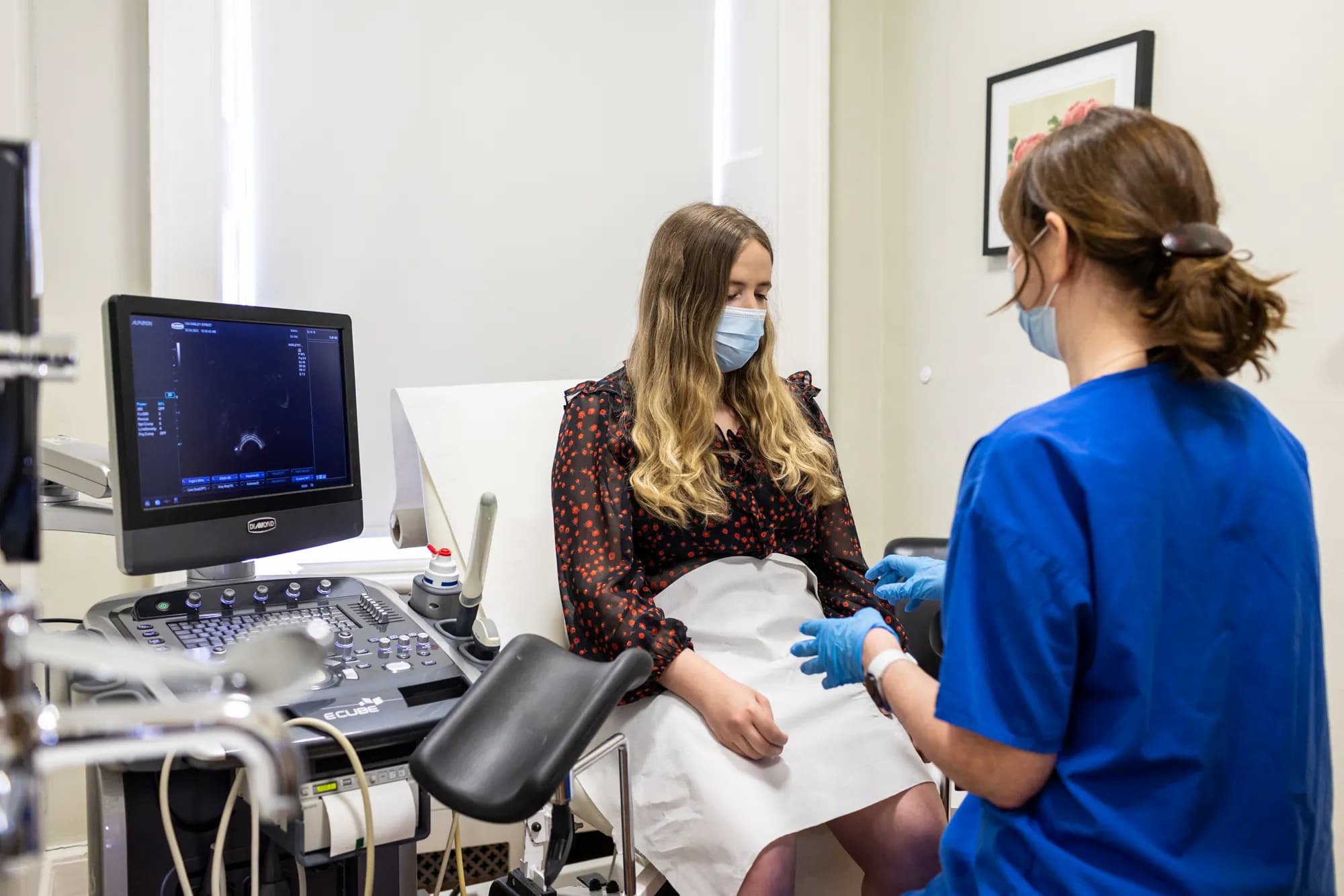
Step 7: Sharing your eggs

Stage 8: Donation and matching

Reciprocal IVF with shared eggs
.jpg?width=1080&height=1080&name=Dr%20Venkat%26PT%20(3).jpg)

Egg sharing and IVF

Let's Talk About What's Right for You
Book a free 15-minute consultation with our New Patient Team. We'll help you understand what's relevant to you and what to expect so you can move forward with confidence.
- Confidential
- No Obligation
- Explore Fertility Options
*Want to book a Doctor's appointment? Get in touch: